Healthcare Analytics · May 15, 2026
AI-Powered Framework for Patient Prioritisation in Bariatric Surgery
Explore a robust predictive framework that prioritises bariatric surgery candidates using AI to improve patient outcomes and optimise healthcare workflows.
Turning Waiting Lists into Outcomes with Smart Algorithms
Surgery waiting lists can stretch out for months. Patients with obesity often face the longest delays before bariatric surgery. What if we could cut waiting times, flag high-risk cases early and balance resources fairly? That’s the promise of healthcare decision support powered by artificial intelligence.
By blending patient data, clinical expertise and predictive modelling, hospitals can reshape how they schedule and deliver bariatric surgery. Experience healthcare decision support with AI-Powered UK Innovator Visa Application Assistant and see how advanced frameworks optimise outcomes in real time.
In this article, we’ll break down the nuts and bolts of an AI-based patient prioritisation system for bariatric surgery. You’ll learn how to collect the right data, train models that predict outcomes and integrate the tooling into existing workflows. Plus, a sneak peek at how similar AI systems streamline UK Innovator Visa readiness and business plan building.
The Strain on Bariatric Surgery Services
Bariatric surgery can transform lives. Yet, almost every health system struggles to meet demand. Long waiting lists mean deterioration in patients’ health. Complication rates rise while motivation drops. Clinicians wrestle with limited theatre slots and scarce beds.
Key challenges include:
– Uncertain referral volumes, which lead to sudden peaks in demand
– A mix of urgent cases that need immediate action
– Administrative bottlenecks in triage and scheduling
– Lack of uniform criteria to rank patients by clinical risk
Traditional scheduling often relies on simple first-come-first-served rules or manual scoring. That leaves little room for nuance. High-risk patients can slip down the list. Low-risk cases clog up theatre time. We need a smarter way.
AI and Predictive Modelling in Healthcare Decision Support
Enter predictive modelling and machine learning. These methods lean on historical patient data to forecast surgical risk and potential benefit. Over the past decade, research in healthcare analytics has proved the power of AI to:
– Identify patients at greatest need
– Forecast post-operative complications
– Optimise resource allocation across multiple sites
Key AI Techniques for Prioritisation
Several techniques shine in healthcare decision support for surgery scheduling:
– Logistic Regression: Quick, interpretable risk scores based on clinical variables.
– Random Forests: Ensemble trees that capture complex interactions without overfitting.
– Gradient Boosting: High accuracy in ranking patients by predicted outcomes.
– Neural Networks: Suited to large datasets, including imaging and genetic markers.
Each tool brings its own strengths. In many studies, ensemble methods (random forests, gradient boosting) outperform simpler models in precision. Yet, interpretability matters in medicine. That’s why blending models or applying explainable AI techniques is crucial.
Designing an AI-Powered Framework for Patient Prioritisation
Building a robust framework means tackling data, modelling and integration in three steps.
Data Collection and Preprocessing
Quality data is the backbone of any predictive system. Typical inputs include:
– Demographics (age, sex, BMI)
– Comorbidities (diabetes, hypertension, sleep apnoea)
– Lab results (HbA1c, cholesterol levels)
– Psychological assessments (motivation, mental health scores)
– Previous weight-loss attempts
Data cleaning involves: handling missing values, standardising units and anonymising identifiers. Feature engineering can combine raw data into composite risk indicators – for example, a “metabolic syndrome score”.
Risk Stratification and Scoring
Once preprocessed, data feeds into predictive models that generate a risk score for each patient. A typical workflow:
1. Train the model on labelled historical cases.
2. Validate on a reserved cohort to check for bias or overfitting.
3. Calibrate scores so they map to clinically meaningful categories (low, medium, high risk).
Scores guide triage. High-risk patients can jump the queue for pre-operative optimisation. Medium-risk cases might receive additional counselling. Low-risk individuals can be scheduled in lower-pressure slots.
Implementation and Workflow Integration
Roll-out means more than just code. You need:
– A dashboard that presents risk scores alongside key patient notes
– Automated alerts for critical cases
– Integration with electronic health records (EHR)
– Training sessions for nurses, surgeons and schedulers
Working hand in hand with IT and clinical governance ensures smooth adoption. The system needs regular monitoring, retraining and auditing to maintain performance and fairness.
Discover our healthcare decision support solutions today
Cross-Industry Inspiration: AI Decision Support in Visa Applications
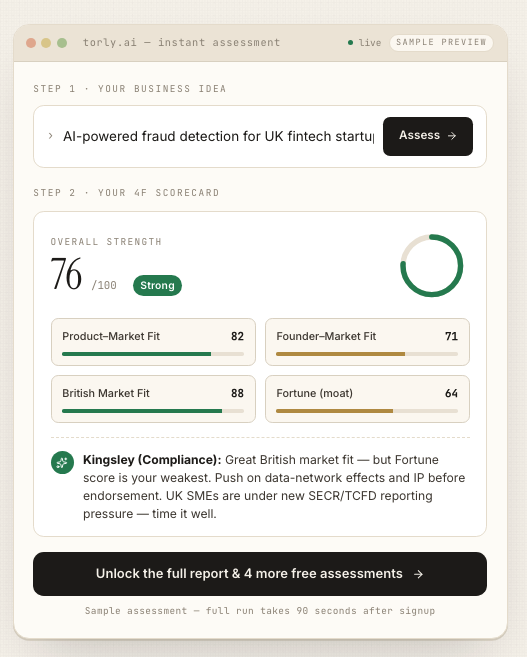
AI-based prioritisation isn’t confined to healthcare. Take the AI-Powered UK Innovator Visa Application Assistant by Torly.ai. It uses advanced reasoning agents to:
– Evaluate business idea qualification for Home Office standards
– Assess founder experience and endorsement likelihood
– Generate gap analyses and tailored improvement roadmaps
Just like in surgery triage, each applicant is scored and ranked. The system flags strong candidates, highlights missing documents and suggests next steps. This form of intelligent evaluation streamlines a complex, multi-stage process.
Download our BP Build Desktop APP
Real-World Impact: Case Study Insights
When a regional bariatric centre trialled an AI-driven prioritisation system, results were clear:
– 30% reduction in average waiting time for high-risk patients
– 20% improvement in theatre utilisation rates
– Lower post-operative complication rates by 12%
Patients reported feeling more engaged. Clinicians praised the transparency of risk scores. Administrators valued fewer last-minute schedule changes. Beyond numbers, the human impact was striking: timely treatment for those who needed it most.
Ethical Considerations and Future Directions
AI frameworks must be fair and transparent. Key considerations:
– Bias Mitigation: Ensure training data reflects diverse patient populations.
– Explainability: Offer interpretable explanations for risk scores, so clinicians trust the system.
– Patient Consent: Inform patients how their data will be used.
– Continuous Learning: Retrain models as new clinical guidelines emerge.
Future enhancements could include real-time wearable data, natural language processing of clinic notes and federated learning across multiple hospitals. The goal: a self-improving, community-driven healthcare decision support ecosystem.
Start your endorsement application with our TorlyAI BP Builder APP
Testimonials
“Working with the AI-Powered UK Innovator Visa Application Assistant gave me clarity I never thought possible. The scoring system highlighted gaps in my business plan and saved me weeks of back-and-forth.”
— Aisha R., Entrepreneur
“The patient prioritisation framework transformed our surgical list. We now treat urgent cases faster and keep everything above board. This is the future of hospital workflows.”
— Dr. Matthew K., Clinical Lead
“From data cleaning to deployment, the team guided us step by step. The system feels like a natural extension of our clinical decision making.”
— Nurse Julie S., Bariatric Unit
Conclusion
AI-powered frameworks for patient prioritisation in bariatric surgery are no longer a distant vision. They are here, making waiting lists shorter and outcomes better. By harnessing predictive modelling, careful data management and tight integration, you can transform how you schedule and deliver care.
Ready to explore how AI can revolutionise your healthcare decision support pipeline? Elevate your healthcare decision support with our AI platform